Anti trypanosomal drugs are those drugs that are used to treat the diseases that are caused by trypanosomes. Before we start to know about these drugs, we should have basic knowledge of trypanosomes. So, define trypanosomes?
What are trypanosomes?
Trypanosomes are flagellate protozoan parasites that occur in the blood and some tissues or tissue fluids of vertebrate animals. The body of the trypanosome is usually leaf-like, elongated shape with a single flagellum containing two nuclei. The majority of trypanosomes are non-pathogenic, but some cause serious diseases in animals together called trypanosomiasis.
Important species of Trypanosoma and their diseases
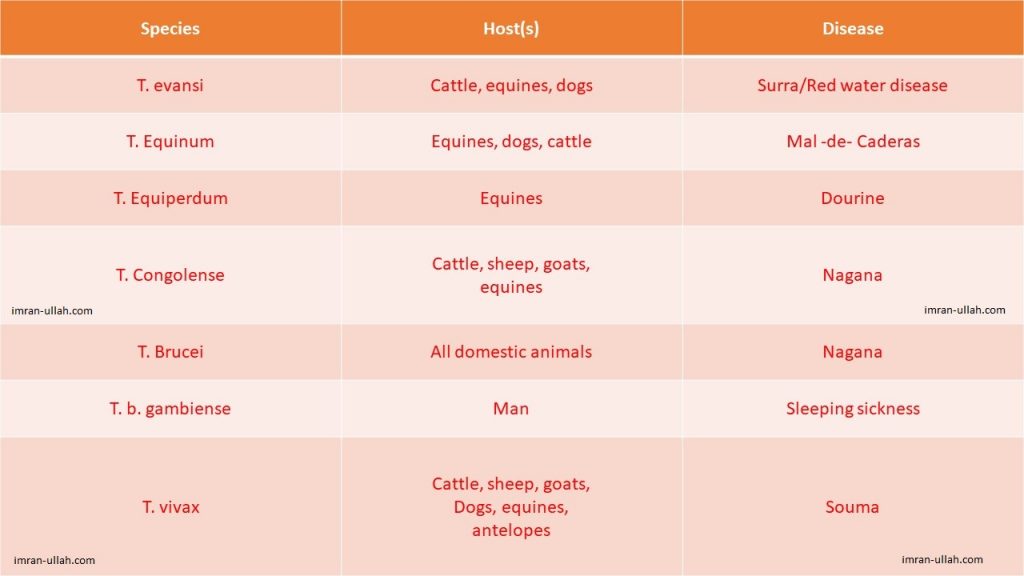
The most commonly encountered specie is T. evansi. It causes red water disease or surra in cattle, horses, and dogs. It is transmitted through biting insects. T. Equinum causes the disease Mal -de- Caderas (disease of the hip) in cattle, horses, and dogs. T. Equiperdum is the cause of a venereal disease called dourine in equines. T. Congolense causes the disease called “Nagana” in cattle, sheep, goat, and equine. T. Brucei also causes “nagana” disease in all domestic animals. In humans, T. rhodesiense, and T. gambiense infect the nervous system and they cause “sleeping sickness”.
What is nagana disease ?
Nagana is a disease caused by trypanosomal protozoa and characterized by lymphadenopathy and anaemia accompanicd by progressive emaciation and, often, death.
Classification of Anti Trypanosomal Drugs
Anti trypanosomal drugs are broadly classified into 6 categories.
- Aromatic diamidines
- Quinapyramine compounds
- Aminophenanthridium compounds
- Carbamide derivatives
- Antimonial compounds
- Dyes
Aromatic Diamidines
Structure
- The basic structure of diamidines contains two guanyl groups separated by an alkyl chain.
- The addition of benzene rings and the substitution of the alkyl chain by an oxygen atom, a dioxyalkyl chain, or ethylene linkage makes a series of trypanocidals of even greater activity.
Mechanism of action
- Inside the trypanosome, the diamidines bind rapidly and irreversibly to DNA or nucleotides and interfere with DNA formation and replication.
- Inhibition of certain enzymes and proteins, interference with aerobic glycolysis, and alteration in uptake or function of polyamines may also be involved in the antitrypanosomal activity.
Examples of Aromatic Diamidines
- Diminazine
- Phenamidine
- Propamidine
- Pentamidine
- Stilbamidine
1. Diminazine
It occurs as an odourless, yellow powder that is
- Relatively soluble in water
- Slightly soluble in alcohol
- Very slightly soluble in ether and chloroform.
As a trypanocidal agent ,it has good efficacy against T.vivax and T.congolense ,but is less Active against T. brucei.
Clinical Uses
- Diminazine is a veterinary drug and is used mainly for the treatment of trypanosomiasis and babesiosis in animals.
- It also possesses some bactericidal action against Brucella and Streptococcus species.
- It is administered by either SC or IM injection.
Side Effects
- Local reactions at the site of injection
- Hypotension
- Tachycardia
- Hepatic and renal impairment
- Hypoglycaemia
2. Phenamidine
It occurs as white odourless crystals that are
- Insoluble in water
- Less soluble in alcohol
- Insoluble in ether and chloroform
Clinical Uses
- Like diminazine, phenamidine is used as a trypanocidal and antibabesial drug.
- It has strong action against T.brucei and T.evansi.
- It is administered subcutaneously.
Side Effects
- Localized reactions at the injection site.
- Mild hypotension.
- GIT disturbances
- Kidney damage
- Hepatic impairment
- Blood dyscrasias
- Hypoglycaemia
Quinapyramine compounds
Quinapyramine
- Quinapyramine sulphate
- Quinapyramine chloride
Quinapyramine sulphate is freely soluble in water whereas quinapyramine chloride is sparingly soluble in water. These two salts are used in combination.
Mechanism of action
- The exact mechanism of action is not known.
- Its action is attributed mainly to inhibition of growth and cell division in the susceptible parasites
Clinical Uses
- In cattle and other species, quinapyramine is administered as a 10% solution by SC injection.
- In horses, it is administered as 5% solution IM.
- It has good efficacy against.
- T. congolense
- T. equiperdum
- T. evansi
- T. equinum
- T. vivax
But it is less efficacious against T.brucei.
Adverse Effects
In younger stock it shows
- Trembling
- Salivation
- Sweating
Whereas , over dosage produces
- Tachycardia
- Tachypnoea
- Collapse
- Death
Aminophenanthridium
Examples
- Homidium (Ethidium)
- Isometamidium
- Pyrithidium
- Dimidium
1. Homidium
Homidium is commercially available as homidium bromide and homidium chloride. Homidium occurs as bitter-tasting dark red crystals.
Clinical Uses
- Homidium is used primarily in veterinary medicine for the treatment and prophylaxis of trypanosomiasis.
- Homidium is active against 1. T.congolense 2. T.vivax
- It is administered by deep IM injection as a single dose. The single dose is both curative and prophylactic for about 1 month.
Adverse Effects
- Localized reaction at the injection site.
- Swelling at the injection site.
- Transient lameness.
2. Isometamidium
- Isometamidium occurs as red crystals and is soluble in cold water.
- It is active against T.congolense, T.vivax, and T.evansi
- It has no activity against other protozoa.
Clinical Uses
- Isometamidium is used for both treatment and prophylaxis of trypanosomiasis.
- As a prophylactic agent, it provides protection against Trypanosoma species for about 2 months.
- The drug is always administered by deep IM injection.
3. Pyrithidium
- Pyrithidium bromide is active against T.vivax, T.congolense, and T. brucei.
- It is administered by IM or SC route as a prophylactic agent.
- A single injection may provide protection against trypanosomiasis for up to 6 months.
4. Dimidium
- It is effective against T.congolense
- It is less active against T.vivax.
- It is inactive against T. brucei and T. evansi.
Carbamide Derivatives
Suramin
Suramin sodium is introduced into the therapy of human trypanosomiasis in 1920. It occurs as slightly bitter-tasting, white or slightly pink or cream coloured powder. It is freely soluble in water.
Mechanism of action
- Suramin enters the trypanosome by endocytosis.
- Free Suramin then acts selectively on some trypanosomal enzymes, particularly trypanosomal cytosolic serine oligopeptidase.
- Suramin also causes damage to intracellular membrane structures of trypanosomes.
Pharmacokinetics
- Suramin is not absorbed after oral administration.
- IM or SC injection often causes severe localized reaction and necrosis of tissues.
- It fails to enter CSF.
- The drug is not significantly metabolized and is eliminated slowly by urine.
Clinical uses
- Suramin has been used in veterinary practice for both curative and prophylactic control of trypanosomiasis.
- In animals, it is generally administered as a 10% aqueous solution by the slow IV route.
- As it is unstable in the air, freshly prepared solutions should be used.
Contraindications
- Suramin is contraindicated in patients that have history of hypersensitivity to it.
- It should not be used in patients with hepatic or renal insufficiency.
Adverse Effects
- Nausea
- Loss of consciousness
Antimonial Compounds
1. Antimony Potassium Tartrate
- Antimony potassium tartrate has been used as an expectorant, a ruminotoric, an anthelmintic, and an antiprotozoal drug.
- It has activity against some blood protozoa including Trypanosoma.
- It is rarely used nowadays because of its adverse effects and the availability of better drugs.
2. Stibophen
- Stibophen sodium has antifilarial, antischistosomal, and antitrypanosomal Properties.
- It is rarely used because of its adverse effects.
Dyes
Trypan Blue and Trypan Red
These compounds are no longer used because they are neither safe nor effective as the modern anti trypanosomal drugs.


